Is Your Skin condition caused by Your Gut – Medical Student Reviews
Last Updated on January 18, 2023 by Aysenur Yashar
Having a clear skin is the dream for most of us. We can talk about the endless amounts of skincare on the shelves and which one is better and which one works, which one reduces wrinkles better. But honestly, with big embarrassment as a medical student, I am sharing that we are forgetting the most important part – a healthy skin comes from a healthy body. So this week’s topic – can your gut actually cause a skin condition?
I am really excited for this blog, I was thrilled when I learnt that I can use my medical knowledge to understand the skin and then skincare better (also help me show off some cool facts to my dermatology professors ahaha).
In this blog you can expect to read how few of the most common skin conditions like acne, rosacea, psoriasis and eczema can be caused actually by a problem in the gut. You will also read some advice about how to approach skin condition from a dermatology professor and a medical student.
Let’s get started!

Why is your gut more important than you think? Can it really influence our skin condition?
If you have been on the quest for a better health you have probably have heard of gut microbiome. Our intestines, especially our colon is colonised by thousands of healthy and good bacteria. We live in symbiosis with them – meaning that we help give them shelter and food and they keep us happy and healthy.
It is not my first time mentioning a microbiome, I have talked about probiotics (which is the juicy food for those good bacteria ) in cosmetics before. Jump to the other blog to learn about the 4 benefits of probiotics in skincare!
It is only recently that the medical community started seeing that changes in this microbiome can be associated with diseases and conditions. These are not just a few rare diseases, we are talking about relatively common conditions like problems in your gastrointestinal system, constipation, inflammation and infections. But the list extends to even anxiety, depression and even the hand tremor in Parkinson’s disease.
So it should come as a no surprise that some of the skin conditions can be due to a problem or unbalance in your gut microbiome.
In medicine, there are many gray zones, and this is one of them, we cannot for sure say which one causes which but there is clear evidence that some conditions like acne, rosacea, eczema come with an unhappy gut boogies.
What is the gut-skin axis?

When we talk about the gut-skin axis we talk about the relationship between the gut and the skin. It has been long known that certain gastrointestinal disease can come accompanied by some skin conditions. Some dermatological conditions can even link to underlying serious gastrointestinal disorders that need emergent treatment.
Currently the scientific literature hypothesised that the gut microbiome – the good bacteria, play a vital role in maintaining our skin health. Following this hypothesis, there were a number of studies which supported this hypothesis.
In one of those studies, 32 volunteers were fed with a probiotic L.paracasei for 2 months. This group showed reduced skin sensitivity and improvement in skin texture. Currently it is thought that the gut can influence the skin by the complicated immune system. But all of the medical community can agree that for a healthy skin a healthy gut is essential
We saw that helping your gut microbiome can have positive effects on our skin, so the reverse should also be true. A damaged gut microbiome should manifest with skin irritation side effects. This is what we observe with many skin conditions from acne to rosacea then to eczema.
Studies show that people with those conditions can have some of the bacterial strains in their gut unbalanced. Oh no, double the problem?
Let’s go deeper into this issue and look at cases one by one.
Acne Vulgaris – should we fix our guts first?
Acne Vulgaris is a chronic inflammatory disease that can affect from 79% – 95% of the Western adolescent population. Making it the most common skin disorder in the Western world. Very surprisingly it is almost absent in some nomadic and hunter-gatherer populations which lead a non-Western lifestyle and diet.
Acne has many factors contributing to its development – some of them include hormonal and immunological state of the patient, over-secretion of sebum, a bacterial strain called C acne, diet, hormonal problems and not regulated levels of insulin like growth factor.
Since the topic is our gut let’s talk about how the gut influences this skin condition. It was long ago suggested that there might be a connection between acne and the gut. In 2018 a study showed that patients suffering from acne vulgaris had a distinctly different microbiome.
They had a decreased levels and diversity of some microbial strains like Firmicutes and increased levels of Bacteroides. So the questions is, so what if there is a connection?
Can diet influence the skin condition – acne vulgaris?

Now that we know the gut flora is changed in those patients, I asked myself is changing our diet effective. Let’s talk science.
Establishing a cause and effect relationship in medicine and science is a very difficult task. This is especially difficult to establish in topics where opinions of experts can vary, such as diet and disease. However epidemiological studies (studies collecting health related information from big populations) give evidence that acne is triggered by western style diet, in which there is high glycemic load. Simply told, western diet is filled with foods that can spike our blood glucose faster.
Epidemiological studies give evidence that acne is triggered by western style diet!
There is a complicated relationship between diet and our bodies. I chose not to dive so much into details but if you want full geeky details just comment below!
So western style diet can trigger acne and change our microbiome for the worse, can probiotics help reverse it?
Well again it is hard to say no or yes easily, but science is working full force on the answer!
Several studies looked into if probiotic supplements would help with acne vulgaris. Daily probiotic consumption especially the ones containing the strain lactobacillus for 12 weeks reduced the inflammatory acne lesions by 30% to 67%. Wow!
Remember how I mentioned the complicated chemical – insulin like growth factor (IGF), this molecule is thought to play a role in the development of acne vulgaris. These studies also showed that the probiotic supplements reduced IGF levels. Yay one stone, two birds!
Rosacea and it’s association with the gut
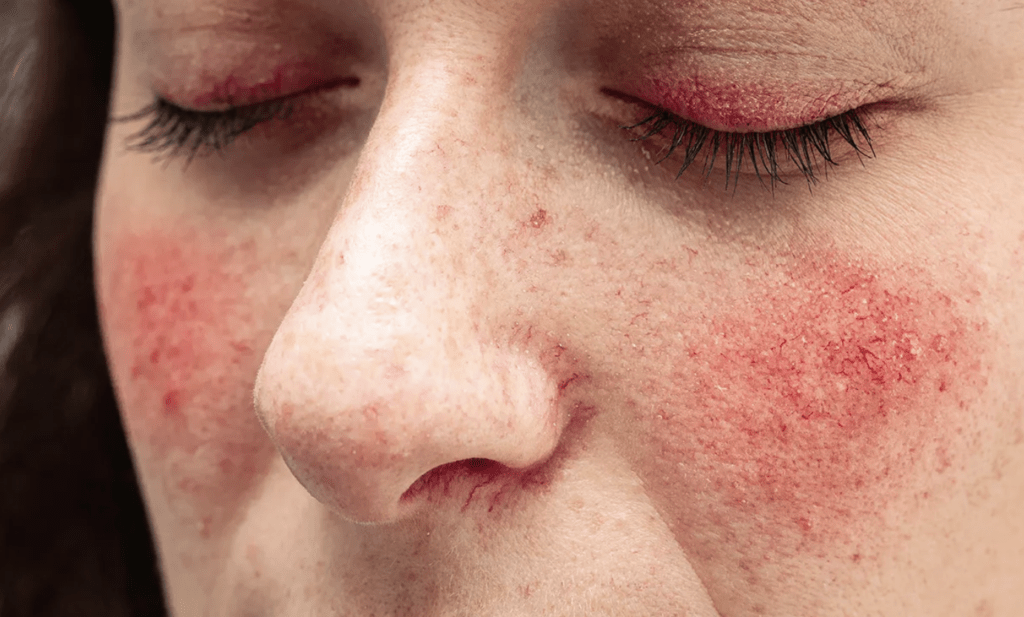
Rosacea is another chronic inflammatory disease which is usually associated with red flushing on the cheeks. Rosacea is a condition that affects up to 15% of the Caucasian population with a sun-sensitive skin type.
So how does this red cheek inducing disease is connected to the gut? The association between the bacteria H. pylori and rosacea has been seen in several studies. Essentially, H.pylori is the bacteria that damages the stomach wall and causes ulcers in the stomach and reflux of acid.
You probably already know someone who suffers from reflux, it is very common and luckily completely treatable!
Another incredible study done nationwide in Denmark included almost 30 000 participants with rosacea, wanted to see if people with rosacea were more prone to having gastrointestinal problems, compared to the rest of the population. And voila, as you can guess, they saw a significant increase in the prevalence of gut problems in people with rosacea. Gut problems from irritable bowel disease to coeliac disease to ulcerative colitis.
It is such a cool study, I cannot wrap my head around that they looked into the whole population!
Very nice geeky facts but how does diet effect this skin condition?
Diet is actually a very important part in triggering rosacea. Although this is an area where more research is needed, a survey done by the National Rosacea Society found that out of 400 patients 78% had needed to change their diet to reduce red flushing.
This means that there are some triggering foods that can increase the red flushes. Which ones are they?
The survey reported that amongst the most common triggers are hot beverages, alcohol especially wine, spices and hot sauces.
So if you have rosacea, unfortunately, you might need to remove some yummy foods from your diet. Consult your doctor for more details. I am sure the best advice will come from them. 🙂

Weren’t we talking about the gut microbiome, would taking probiotics help with rosacea?
Currently how the gut microbiome affects rosacea is an area that needs more research and there is no data specifically showing a cause and effect relationship. But having in mind the inflammation relieving effects of probiotics we can guess that they might work for rosacea. But as of now, this only remains as a guess
However, on the lighter note, let’s get to the juicy part, what to do to relieve your skin condition or avoid it in general?
Advice from a dermatologist and a medical student
I hope this was fun for you because I loved learning about the gut-skin connection! Now that we are equipped with all those geeky medical facts, what do we do. Do we start taking probiotics like crazy with the hopes that it will make our skin brighter and healthier?
I actually do not know, there seems to not be an easy fix to those serious skin conditions. So I asked the professionals!
In the beginning of the week I was at my dermatology rotation, in between seeing patients, I was lucky enough to have a very curious conversation with my professor.

After telling her everything I have learnt while writing this blog, I got more confused, so what diet advice do we give to rosacea and acne vulgaris patients.
I was not expecting this answer but I was not surprised – she said we DO NOT recommend diet changed, but a LIFESTYLE change!
This includes changes to your diet, switching to Mediterranean style of diet, exercising, not smoking, not drinking and avoiding stress as much as possible!
I know it sounds stupid and silly especially coming from health care workers, but everyday I spent in the hospital I realise that lifestyle changes can not only make you free of your skin condition but it can save lives!
Stay tuned for more on skincare and nutrition, more tips and tricks from a medical student!
If you are wondering what applying probiotics would do to your face, this read is a must for you! If you are also on the quest for going all natural and organic in your skin care routine, here are clean 5 brands that are worth your money!
References
- O’Neill, C.A., Monteleone, G., McLaughlin, J.T. and Paus, R. (2016), The gut-skin axis in health and disease: A paradigm with therapeutic implications. BioEssays, 38: 1167-1176. https://doi.org/10.1002/bies.201600008
- Gueniche A, Philippe D, Bastien P, Reuteler G, et al. 2014. Randomised double-blind placebo-controlled study of the effect of Lactobacillus paracasei NCC 2461 on skin reactivity. Benef Microbes 5 : 137–45.
- De Pessemier B, Grine L, Debaere M, Maes A, Paetzold B, Callewaert C. Gut–Skin Axis: Current Knowledge of the Interrelationship between Microbial Dysbiosis and Skin Conditions. Microorganisms. 2021; 9(2):353. https://doi.org/10.3390/microorganisms9020353
- Shivani Sinha, Gloria Lin, Katalin Ferenczi, The skin microbiome and the gut-skin axis, Clinics in Dermatology, Volume 39, Issue 5, 2021, Pages 829-839, ISSN 0738-081X, https://doi.org/10.1016/j.clindermatol.2021.08.021.
- Egeberg, A., Weinstock, L., Thyssen, E., Gislason, G. and Thyssen, J. (2017), Rosacea and gastrointestinal disorders: a population-based cohort study. Br J Dermatol, 176: 100-106. https://doi.org/10.1111/bjd.14930
- Andrea Parodi, Stefania Paolino, Alfredo Greco, Francesco Drago, Carlo Mansi, Alfredo Rebora, Aurora Parodi, Vincenzo Savarino, Small Intestinal Bacterial Overgrowth in Rosacea: Clinical Effectiveness of Its Eradication, Clinical Gastroenterology and Hepatology, Volume 6, Issue 7, 2008, Pages 759-764, ISSN 1542-3565, https://doi.org/10.1016/j.cgh.2008.02.054.v
- Drake L. Hot sauce, wine and tomatoes cause flare-ups, survey finds Rosacea.org
- Weiss E, Katta R. Diet and rosacea: the role of dietary change in the management of rosacea. Dermatol Pract Concept 2017;7(4):31-37. DOI: https://doi.org/10.5826/dpc.0704a08





